In 2026, the question for healthcare founders has shifted from “Should we build an app?” to “How do we survive the ecosystem?”
The market is no longer impressed by basic HIPAA compliance or standard video calls. Those are now the bare minimum, the “entry fee” for a seat at the table. The real work now lies in designing intelligent healthcare systems that reduce clinical friction, preserve human trust, and quietly integrate into care delivery without overwhelming the people they are meant to serve. As healthcare technology matures, the questions shaping the next generation of platforms are no longer technical alone — they are ethical, experiential, and structural.
The Healthcare Industry Talent Deficit and Need for Technology
“Technology has always been the silent backbone of healthcare, but in 2026, it’s no longer just about ‘improvement’. It’s about survival. The math simply doesn’t add up anymore. The latest AAMC projections show a physician shortage gap of up to 86,000 doctors by 2036. While legislative efforts are underway to add residency slots, the immediate solution isn’t more people; it’s more leverage. This is where the ‘Agentic AI’ we discussed earlier moves from a luxury to a logistical necessity.”
The Burden of the “Avoidable” Visit
The strain on our hospitals isn’t just a lack of staff; it’s a misallocation of their time. 2024 data from NCQA confirms that up to 60% of all ED visits remain non-urgent and potentially unnecessary.
In a world where medical cost trends are hitting 8.5% inflation in 2026, these avoidable encounters are more than just an inconvenience—they are a multi-billion dollar leak in the system.
The $1 Trillion Opportunity
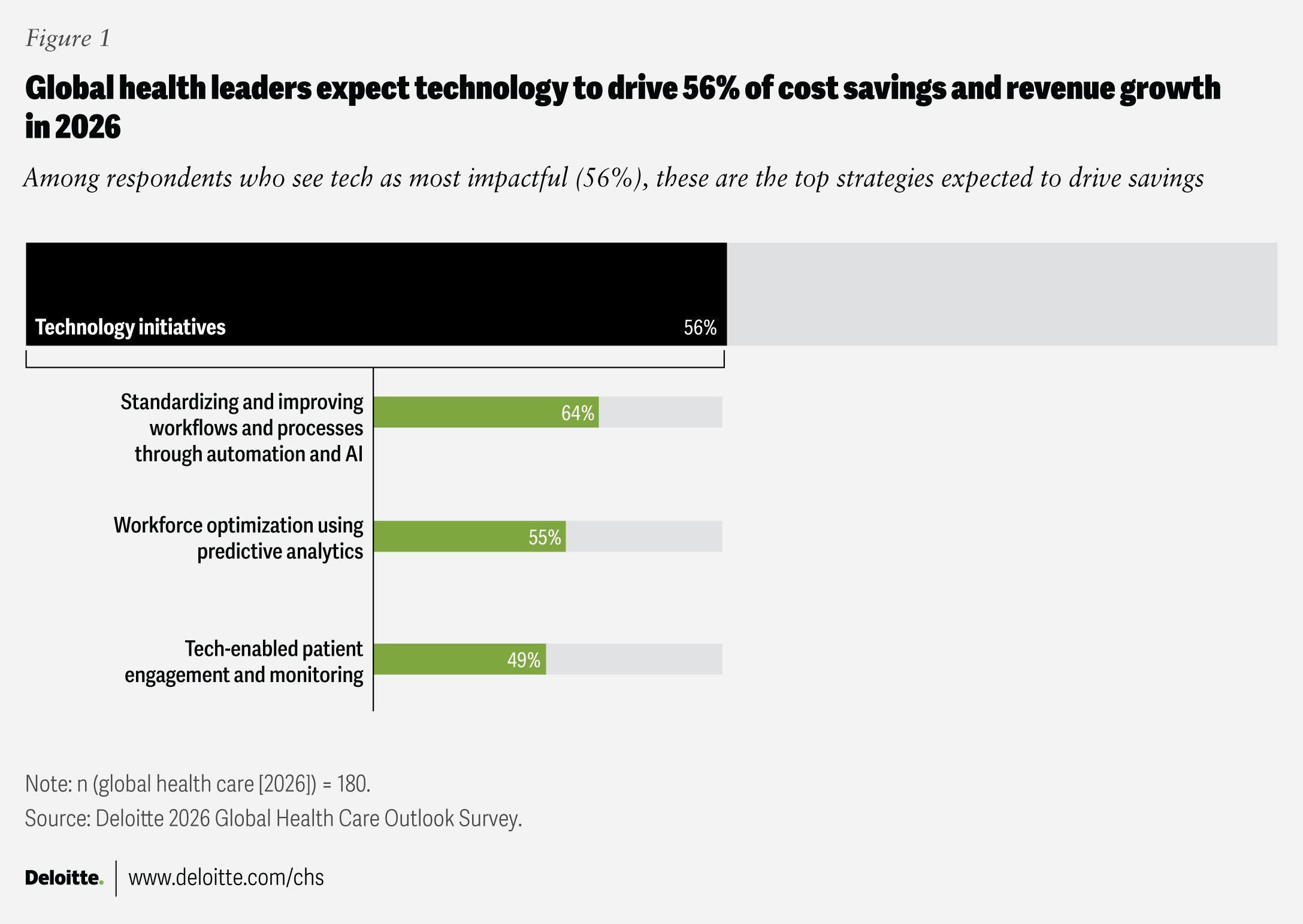
If we can cut unnecessary visits by half, we don’t just save the $5.2 billion annually cited in earlier years. According to PwC’s 2025 “Breakthrough” report, there is a $1 trillion opportunity to shift healthcare spending from “outdated cost pools” (like administrative overhead and brick-and-mortar facilities) into next-generation models like AI-enabled intake and hospital-at-home programs.
The 2026 Takeaway: To capture this value, your app cannot just be a “portal.” It must be a tool for proactive prevention.
This guide cuts through the noise to show you exactly how to build a healthcare product that scales, stays compliant, and most importantly, becomes an indispensable part of the clinical workflow.
Step 1: The Clinical Discovery & Risk Profiling
Before code, before design, before funding projections, you first define the app’s medical intent. In healthcare, your product is not just software; it is a clinical intervention with consequences. That means answering a deceptively simple question early: what exactly is the medical purpose of this application, and what level of clinical responsibility does it carry?
By 2026, the first fork in the road is whether your product sits in the relatively lighter “wellness” category or qualifies as Software as a Medical Device (SaMD). That classification determines everything that follows – regulatory obligations, validation requirements, liability exposure, documentation effort, and often 3–5x differences in development cost and timeline. A symptom tracker and an AI-powered diagnostic tool may share similar interfaces, but they live in completely different regulatory worlds.
Equally important is mapping the real-world clinical workflow, not the imagined one. Healthcare systems reject products that optimize for one stakeholder while burdening another. The patient experience, provider experience, and institutional workflow must all improve simultaneously.
A strong discovery phase typically includes:
- Dual user journey mapping
- Patient journey: onboarding, symptom reporting, data sharing, follow-up
- Provider journey: data interpretation, documentation load, clinical decision flow
- Clinical gap analysis — identifying where current workflows fail and where technology meaningfully reduces friction
- Risk classification and regulatory pathway planning
- Stakeholder interviews with clinicians, nurses, administrators, and patients
- Failure scenario mapping (misdiagnosis risk, data errors, delayed alerts)
Consider a simple teleconsultation platform: if it saves patients 15 minutes but forces doctors to manually enter structured notes after every session, adoption collapses. Clinical discovery ensures the system creates net value across the ecosystem, not just a pleasant user interface.
Industry surveys show that nearly 70% of healthcare IT projects fail due to workflow mismatch rather than technical failure, which makes this phase less optional strategy and more survival mechanism.
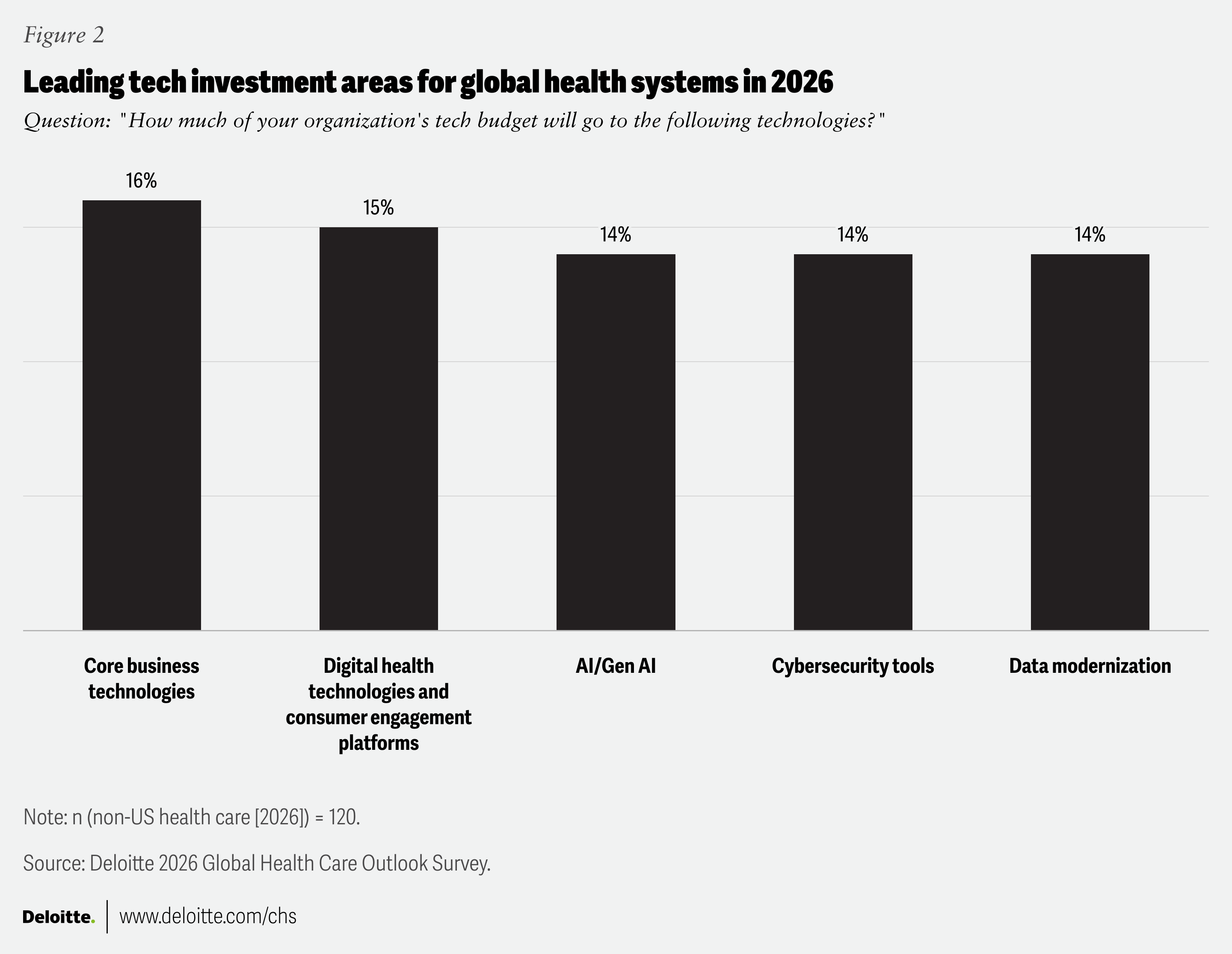
Step 2: Compliance-First Architecture
Healthcare software is built around trust, and trust is engineered, not patched later. In most industries, security arrives as a final checklist item. In healthcare, it shapes the architecture from day one because patient data is among the most sensitive information any system handles.
Compliance-first architecture means designing infrastructure where privacy, traceability, and accountability are structural properties of the system. Data protection laws, auditability requirements, and breach liabilities influence how services communicate, how identities are verified, and how data flows across the platform.
This phase focuses on:
- Identity-first security design
- Role-based and attribute-based access control
- Multi-factor authentication for clinicians and staff
- Zero-trust architecture — no implicit trust between services, users, or devices
- End-to-end encryption
- Data at rest
- Data in transit
- Data in use (increasingly critical with AI workloads)
- Audit logging and traceability — every data action must be attributable
- Consent management frameworks — explicit patient control over data sharing
- Secure infrastructure design (segmented environments, isolated workloads)
The technical requirement is straightforward: the system should assume that breaches will be attempted and should remain resilient even when components fail.
Large hospital systems handling millions of patient records rely on strict data governance models — for instance, platforms integrating with systems like Epic Systems must maintain strict authentication and audit trails to access electronic health records. Your application needs to operate at comparable standards if it touches clinical data.
Healthcare breaches are expensive. Period. Global studies estimate the average cost of a healthcare data breach at $10 million+ per incident, consistently the highest across industries. Compliance-first architecture protects users, institutions, and your product’s long-term viability.
Step 3: Rapid Prototyping & the UI/UX Stress Test
Healthcare software is rarely used under ideal conditions. Patients may be anxious, in pain, elderly, or unfamiliar with technology. Clinicians operate in high-pressure environments with constant interruptions. This makes usability not just a design preference but a clinical safety requirement.
Rapid prototyping allows teams to validate usability before expensive engineering begins. Instead of static mockups, teams create interactive prototypes that simulate real workflows and expose friction early.
Healthcare UX design prioritizes:
- Accessibility-first interfaces
- Large touch targets for motor limitations
- High contrast for low-vision users
- Clear typography and simplified navigation
- High-cognitive-load environments
- Minimal decision steps
- Information hierarchy for quick scanning
- Reduced documentation burden
- Error prevention and recovery flows
- Voice or assisted input for limited mobility scenarios
Real-world testing reveals insights that design teams cannot predict. For example:
- An elderly patient struggling with small form inputs
- A nurse missing a critical alert buried inside a dashboard
- A consultation flow requiring too many steps during emergencies
Prototypes are deliberately stress-tested with real users — patients, caregivers, and clinicians — to surface these issues. Studies from global health usability research suggest that improving interface clarity alone can reduce clinical data entry errors by up to 40%, demonstrating how design decisions directly impact care quality.
Step 4: The Core Build & Integration
Once the clinical logic, security architecture, and user experience are validated, the system moves into full-scale development. This stage involves building the actual product, but in modern healthcare, the challenge is rarely building features alone. The real work lies in integrating with the existing healthcare ecosystem.
A contemporary build strategy typically includes:
- Cross-platform development frameworks for faster deployment across devices
- Cloud-native or serverless backends for scalability and reliability
- Modular microservices architecture for independent feature evolution
- FHIR-based interoperability layers to exchange clinical data with hospital systems
- AI-enabled decision support features
Interoperability is the defining challenge of healthcare technology in 2026. Hospitals operate complex electronic health record systems, diagnostic tools, billing platforms, and legacy infrastructure. A new application must communicate with these systems seamlessly or risk becoming an isolated tool with limited value.
Key integration goals include:
- Accessing patient histories securely
- Writing clinical notes into hospital systems
- Synchronizing lab results and diagnostic data
- Supporting standardized health data formats
- Maintaining real-time communication with providers
AI features increasingly move beyond analytics into action. Modern healthcare apps may:
- Flag abnormal lab results automatically
- Prioritize patient queues based on risk signals
- Assist clinical triage decisions
- Monitor chronic conditions using predictive models
According to the World Health Organization, AI-driven decision support is expected to assist in up to 30% of routine clinical decision workflows by 2030, which explains why intelligent automation is rapidly becoming a core product capability rather than an optional add-on.
Step 5: Rigorous Testing & Clinical Validation
In healthcare software, testing is not just about functionality — it is about safety, reliability, and legal defensibility. A minor software bug in another industry may cause inconvenience; in healthcare, it can affect diagnosis, treatment, or patient outcomes.
Testing at this stage is deliberately exhaustive and includes scenarios that rarely occur but carry high risk.
Typical validation activities include:
- Edge-case testing
- Network failures during consultations
- Corrupt or incomplete device data
- Concurrent access conflicts
- Clinical workflow simulation — ensuring accuracy under real conditions
- Performance testing under peak loads
- Penetration testing to identify security vulnerabilities
- Compliance audits to validate regulatory adherence
- Data integrity verification — ensuring medical records remain accurate and traceable
Traceability becomes especially critical. Every action, from data access to algorithmic decision-making, must be recorded and auditable. This provides accountability, supports regulatory review, and protects healthcare institutions from liability.
Clinical validation may also involve pilot studies or expert review panels to ensure the system behaves consistently with accepted medical standards before broader deployment.
Step 6: Controlled Launch & Continuous Feedback Loop
Healthcare products rarely succeed through mass launch strategies. Instead, they enter real-world environments gradually, where performance can be monitored closely and risks contained.
A controlled launch typically begins with:
- Pilot deployments in a single clinic or hospital department
- Limited patient cohorts for early testing
- Performance monitoring dashboards
- User feedback collection from clinicians and patients
- Operational workflow adjustments
Post-launch monitoring focuses on system reliability and model performance, especially for AI-driven features. Over time, predictive systems can drift — their accuracy may degrade as patient populations or usage patterns change. Continuous monitoring ensures clinical recommendations remain safe and effective.
Successful healthcare products evolve continuously through:
- Ongoing compliance updates
- Feature refinement based on clinical feedback
- Performance optimization
- Model retraining and validation
- Expansion into new use cases
Healthcare software is less a finished product and more a continuously maintained clinical system.
The 2026 Takeaway: It’s a Marathon, Not a Sprint
Building a healthcare application is a long-term commitment to a living system that operates within clinical, legal, and human realities. It demands far more than engineering capability — it requires an understanding of clinical workflows, regulatory landscapes, data ethics, and patient experience.
The teams that succeed treat healthcare software as infrastructure for care delivery rather than a standalone digital product. They validate continuously, design cautiously, and improve relentlessly — because in healthcare, trust is built slowly and lost instantly.


